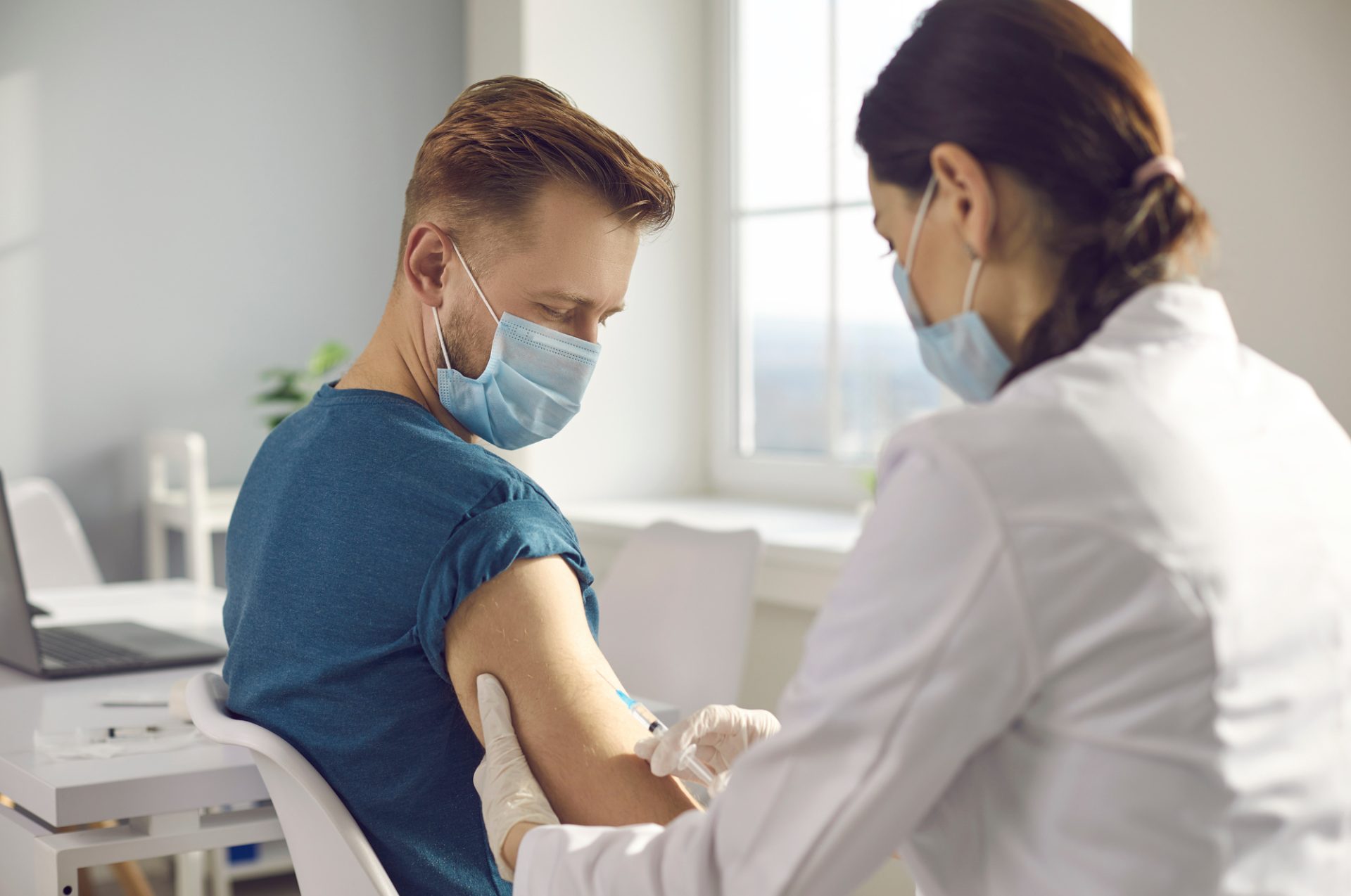
The inefficient and error-prone paper collection method was the norm as far as clinical trials were concerned… not until the early 2000s happened. So, what sort of phenomenon blew it out of the water? Electronic data capture (EDC) is the name. Considered an offshoot of remote data entry technology, it has enabled studies to proceed faster and more smoothly, all while ensuring superior data quality. It’s safe to say that modern treatments—and the patients they cured—owe their creation to this tech.
One study shows that roughly three-quarters of clinical studies use a wide range of EDC platforms. This speaks tons about how convenient the system is. Nevertheless, experts warn that utilizing too many systems can lead to data quality issues and untenable cost increases. Other stumbling blocks complicating their usage are the decentralization of trials and the shift in focus to patient welfare, to name some.
A number of industry professionals advise against employing multiple EDC systems. Despite that, such a practice is unlikely to fall out of favor anytime soon. For a treatment to be approved for public use as quickly as possible, trials must collect and analyze more data in a limited timeframe. A good start may be to harness the right technology.
Outdated mechanism
Absolute data accuracy is impossible. Perfection doesn’t exist in this sphere. However the introduction of EDC in clinical trials was a step in the right direction. It got rid of most of the issues plaguing its paper-based predecessors; the repetitiveness of data entry and delays in discovering discrepancies became things of the past.
The first few years after its rollout transformed healthcare data collection and analysis through reduced research times and costs. There’s virtually any doubt about its growing role in clinical trials moving forward.
Anyhow, experts point out that the system has struggled to keep up with the growing complexity of clinical trials. Why is this so? Much of today’s data is unstructured, sourced from wearable devices and health apps, which EDC isn’t designed to work with. This can be a serious limitation for trials that need nonstop, real-time data gathering or those conducted through telehealth. Bridging this gap often requires human-in-the-loop clinical data abstraction to normalize unstructured notes, PDFs, and device feeds into analysis-ready variables and trial endpoints. For readers seeking a primer on workflows, governance, and quality controls behind these services—e.g., trained abstractors, standardized definitions, dual-review, and audit—see what is data abstraction. When paired with EDC and eSource tools, abstraction can reduce duplication between EHR and case report forms, improve data quality, and accelerate query resolution across multi-EDC environments.
For EDC to remain relevant amid changes in medical research, it’s important to make it work alongside current advancements. With the help of clinical trial software, structured and unstructured data can be collated into a single access point. What’s more, the software can also detail entries such as collection methods and usage history.
Siloed development
The truth is that getting different systems to work together is easier said than done. For one, their development was initiated independently, and EDC is no exception. See, an average trial can have dozens of data management platforms, each with its own skillset requirements and system builds. Think of it as having a specially designed spoon or fork for every type of dish. Yes, things can get THAT complicated.
This lack of integration often leads to duplication. By one estimate, EDC and electronic health records (EHRs) have around a sizeable fraction of their data duplicated, which translates to millions in unnecessary research expenses and time that could’ve been allocated to refining the treatment.
With the industry realizing this shortcoming, it has led to the development of integrated technologies. One notable example is EHR2EDC, an umbrella term for projects involving the creation of a mechanism that automatically retrieves EHR data in hospitals. While such endeavors have been ongoing for decades, it’s only with the current tech that the system has become more feasible.
Fortunately, interoperability may become less of an issue as technology progresses. Given the problems discussed so far, the industry can expect the various platforms to be more enmeshed over time. It pays to develop the mindset that EDC alone won’t be enough as early as now.
Clinical trial decentralization
Conventional clinical trials take place in a hospital or medical research facility, so that means researchers require participants to make the journey occasionally. While it isn’t a problem for those living in metropolitan areas, the same can’t be said for seven out of 10 subjects residing over two hours away from the nearest trial site. Imagine the struggle!
Also, in the midst of recent global events, clinical trials are under pressure to decentralize testing by harnessing telehealth and other digital platforms. Of course, full decentralization won’t be possible in the meantime, so the vast majority will most likely be a hybrid setup. Thus, medical research can still continue amid shutdowns and other similar events.
Onsite testing is a more advantageous environment for legacy EDC systems as they can collect and assess data from patient records. In spite of that, the data suddenly becomes suspect when the primary source is a conversation with the patient whose statements can’t be verified through direct testing. Are the extra steps necessary for validation? Yet another burden for the researchers.
All this doesn’t imply that EDC is ill-suited for data collection and analysis in decentralized clinical trials (DCTs). It can still receive valid data from health monitoring apparatuses worn or used by the patient.
Screening participants by setting inclusion and exclusion criteria before the trial is sensible. It’s a practice that lowers the risk of injury during the study and reduces the burden of sorting through immense amounts of irrelevant data.
Conclusion
EDC will remain the primary means of healthcare data gathering and analysis in the following years. There’s no stopping its domination despite all the challenges it’s facing. Then again, the said technology has to keep up with the rapidly changing and sometimes erratic nature of clinical trials. Otherwise, it risks sharing the same fate as the method it succeeded, and this is only possible with an integrated platform that goes beyond EDC.
Kyle Lewis is a seasoned technology journalist with over a decade of experience covering the latest innovations and trends in the tech industry. With a deep passion for all things digital, he has built a reputation for delivering insightful analysis and thought-provoking commentary on everything from cutting-edge consumer electronics to groundbreaking enterprise solutions.